Last spring, a group of 14-year-old girls sat in silence on metal chairs in a government health center in New Delhi, their braids swinging as they browsed through their phones. With practiced efficiency, a nurse went from one to the next, swabbing arms, giving the HPV vaccine, and applying tiny beige bandages. It was a disciplined, almost everyday scene. Nevertheless, something important was taking place in that room, something that might not become completely apparent for decades.
In many respects, HPV vaccination is a gradual public health measure. It guards against infection with some high-risk human papillomaviruses, particularly HPV 16 and 18, which together account for most cervical cancers globally. Since the vaccine was first introduced in 2006, the body of evidence supporting it has grown, making it hard to reject.
Still, there is skepticism.
| Category | Details |
|---|---|
| Vaccine Name | HPV (Human Papillomavirus) Vaccine |
| First Approved | 2006 |
| Target | High-risk HPV types (including 16 & 18) |
| Diseases Prevented | Cervical, anal, penile, throat and other cancers |
| Recommended Age | 9–14 years (routine), up to 26 years |
| Dose Schedule | Single dose (WHO updated guidance) or 2–3 doses depending on age |
| Global Reach | Introduced in 150+ countries |
| Annual Cervical Cancer Cases (India) | ~125,000 |
| Annual Cervical Cancer Deaths (India) | ~75,000 |
| CDC Information | https://www.cdc.gov/hpv/vaccines |
| WHO Guidance | https://www.who.int/teams/immunization-vaccines-and-biologicals |
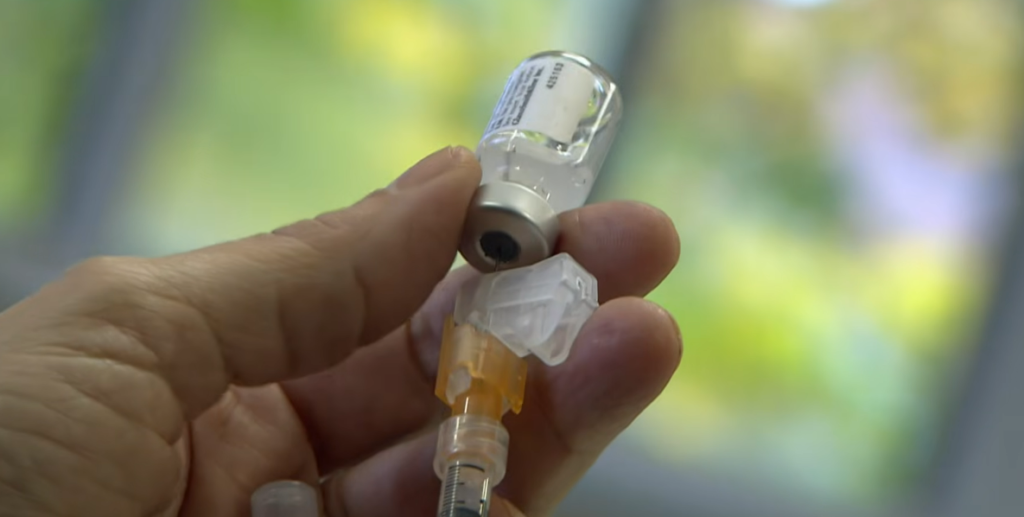
The government of India, where cervical cancer is still the second most common cancer among women, is launching a national campaign aimed at girls aged 14 years. The reasoning is simple: get vaccinated before being exposed. According to revised WHO guidelines, adolescence provides the strongest immune response, resulting in long-lasting protection with just one dose. However, public confidence does not always follow from clear policies.
It’s difficult to overlook how the discussion surrounding HPV vaccination touches on more general concerns about safety, sexuality, and governmental regulations. In conservative communities, the HPV vaccine can occasionally cause discomfort because it is sexually transmitted. Parents are hesitant. There are rumors. Doubt spreads more quickly than facts on social media.
However, the data has a more subdued, steady voice.
Since the vaccine’s launch, the incidence of cervical cancer in young women in the US has dramatically decreased. Declines have been more pronounced in states with higher vaccination rates. In younger age groups, some have reported reductions of over 50%. It seems as though the vaccine is accomplishing its goal as you watch those graphs go down.
Perhaps the most striking example is provided by Australia. The nation witnessed sharp declines in HPV infections and precancerous lesions following the introduction of the HPV vaccine in 2007 and its expansion to boys in 2013. According to public health experts, Australia may be able to eradicate cervical cancer as a public health issue in a matter of decades. In the past, such a statement sounded aspirational. It sounds realistic now.
The stakes are very high in India. Every year, about 125,000 women receive a cervical cancer diagnosis, and about 75,000 of them pass away from the disease. There is no abstraction in these figures. They stand for wage earners, mothers, daughters, and lives that have been disrupted. A well-run vaccination campaign might be able to gradually slant that curve in the opposite direction, which would lessen the burden on overcrowded oncology wards as well as mortality. However, execution is crucial.
Pilot programs have already shown high uptake in a few states. During its rollout, Sikkim’s coverage rates exceeded 95 percent. In a few districts, Punjab reported similar success. However, logistical challenges for national programs include parental consent, digital booking systems, cold chain management, and rural access. It is execution, not science, that can cause vaccination campaigns to fail.
Another problem is complacency. The percentage of teenagers who have received at least one dose of the HPV vaccine has plateaued in some areas of the US, at about 78%. Public health officials are concerned that progress may be undermined by disinformation and shifting political tides. It’s still unclear if new advisory reviews in some nations will merely restate proven safety data or spark needless controversy.
Hundreds of millions of doses have been given worldwide, and the safety record is still strong. It is a non-live vaccine. It doesn’t infect people with HPV. Soreness, exhaustion, and the occasional fainting in adolescents—which is not unusual with vaccines—are the most common side effects. Rarely do severe reactions occur. That evidence has been examined numerous times. However, trust is brittle.
One feels both hope and hesitancy as they watch a mother nervously adjust her scarf as she walks her daughter into a vaccination room. It takes a few seconds to inject. Years pass during the protection. However, the choice seems more significant than the present.
The HPV vaccine is also a part of a larger social change. In the past, screening methods such as Pap smears, follow-ups, and early detection were crucial to the prevention of cervical cancer. By preventing infection before aberrant cells even form, vaccination alters that equation. It shifts the conflict upstream.
Regardless of vaccination status, some critics contend that routine screening should always be a top priority, and they are correct. Although vaccination lowers risk, it does not take away from the need for caution. There are rarely absolutes in public health. It provides probabilities.
The trajectory is encouraging, though.
Over 150 nations have included HPV vaccination in their national immunization programs. Access and affordability are being improved by single-dose approaches, especially in low- and middle-income countries. Global health investors, including collaborations like Gavi, appear to think that consistent funding could hasten coverage, especially in areas with the greatest burden.
It is difficult to deny that the HPV vaccine holds a unique place in medicine as a preventative measure that, with a straightforward injection administered during adolescence, can significantly lower the risk of developing a serious cancer. Interventions are rarely that straightforward.
However, progress hinges on an intangible: the willingness of all.
